Ovarian Cancer: What to Know
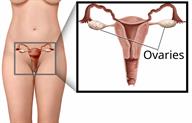
Ovaries are the parts of the female body that make eggs and hormones. They're on each side of your uterus. Growths of cells that aren't normal called tumors can form on your ovaries. These tumors may be benign, which means they're not cancer. Or they may be malignant, which means they are cancer.
Ovarian cancer is when you have cancerous tumors on one or both of your ovaries.
The types of ovarian cancer include:- Epithelial. This is when the tumors form on the outer surface of the ovary. It's the most common type.
- Germ cell. This is when the tumors grow in the part of your ovary that makes eggs.
- Stromal cell. This is when the tumors grow in the part of your ovary that makes hormones.
Cancerous tumors may spread to other parts of your body.
What are the causes?
The exact cause of this cancer isn't known.
What increases the risk?
You may be more likely to get this type of cancer if:- You're 50 years of age or older.
- You carry a changed gene, also called a gene mutation, such as BRCA1 or BRCA2.
- You or someone in your family has had:
- Endometrial cancer.
- Colon cancer.
- Breast cancer.
- Ovarian cancer.
- You get pregnant for the first time at 35 years of age or older.
- You've never been pregnant.
- You've taken some type of hormone replacement therapy.
- You're overweight.
- You have endometriosis. This causes tissue from your uterus to grow outside the uterus.
What are the signs or symptoms?
In the early stages, the cancer may not cause symptoms. As the cancer grows, you may have:- Problems with your belly, such as:
- Bloating.
- Swelling.
- A lump.
- Pain.
- Weight loss or tiredness that you can't explain.
- Pain and pressure in your back.
- Pain or pressure in the spot between your hip bones. This area is called your pelvis.
- Lack of hunger or feeling full more quickly when eating.
- An upset stomach or trouble pooping.
- Having to pee often or feeling pressure on your bladder.
- Pain during sex.
How is this diagnosed?
Ovarian cancer may be diagnosed based on your symptoms, medical history, and an exam. You may also have tests. These may include:- A biopsy. This is when a small piece of tissue is removed from your ovary for testing.
- Imaging tests, such as:
- An ultrasound.
- An X-ray.
- A CT scan.
- An MRI.
- A PET scan.
- Blood tests. These may include genetic testing, which is a type of test that looks for changes in your genes.
Your cancer will be tested, or staged, to see how serious it is and how much it has spread.
How is this treated?
Treatment depends on the type and stage of the cancer. You may need:- A surgery called an oophorectomy. During this surgery:
- The ovary is removed.
- Other tissues may be taken out, such as your fallopian tube.
- Your uterus and nearby lymph nodes may also need to be removed in some cases.
- Medicines to kill the cancer cells. These may include chemotherapy or targeted cell therapy.
- Hormone therapy. This uses hormones or hormone-blocking medicines to fight cancer cells.
- Immunotherapy. This uses medicines to help your body's defense system (immune system) fight cancer cells.
Follow these instructions at home:
Medicines
-
Take over-the-counter and prescription medicines only as told by your health care provider.
-
Work with your provider to manage side effects of treatment.
General instructions
-
Do not use any products that contain nicotine or tobacco. These products include cigarettes, chewing tobacco, and vaping devices, such as e-cigarettes. If you need help quitting, ask your provider.
-
Eat healthy meals often.
-
Return to your normal activities as told by your provider. Ask your provider what activities are safe for you.
-
Keep all follow-up visits. Your provider will watch your condition closely. They may change your care plan over time.
Where to find support
Think about joining a support group for people who have or have had cancer.
Where to find more information
-
American Cancer Society: cancer.org
-
National Cancer Institute: cancer.gov
Contact a health care provider if:
-
You have a fever or chills.
-
You can't follow your treatment plan.
-
You can't take a medicine you were given.
-
There are changes in how you pee or poop.
-
You have any symptoms or changes that worry you.
This information is not intended to replace advice given to you by your health care provider. Make sure you discuss any questions you have with your health care provider.

